Top 10 UV Disinfection Systems for Hospitals to Ensure Patient Safety?
The importance of effective disinfection in hospitals cannot be overstated. With healthcare-associated infections on the rise, adopting advanced techniques like UV disinfection systems has become crucial. A recent report by the Centers for Disease Control and Prevention states that nearly 1 in 31 hospital patients has at least one healthcare-associated infection. This alarming statistic highlights the urgent need for reliable disinfection solutions.
Experts in the field, such as Dr. Emily Reynolds, a leading researcher in hospital sanitation, emphasize the role of UV disinfection systems in combating these infections. She states, "The implementation of UV disinfection systems in hospitals drastically reduces pathogen load." These systems offer a proactive approach to infection control, providing an extra layer of safety for patients and staff alike. However, some facilities still overlook the integration of such technologies due to budget constraints or lack of awareness.
Investing in UV disinfection technology is not without challenges. Hospitals must consider the initial costs, training staff, and ongoing maintenance. These factors can lead to hesitation in adoption. Yet, as more institutions recognize the benefits, the balance may shift towards a more standard practice in healthcare settings. The case for UV disinfection systems in hospitals is compelling and deserves serious consideration.
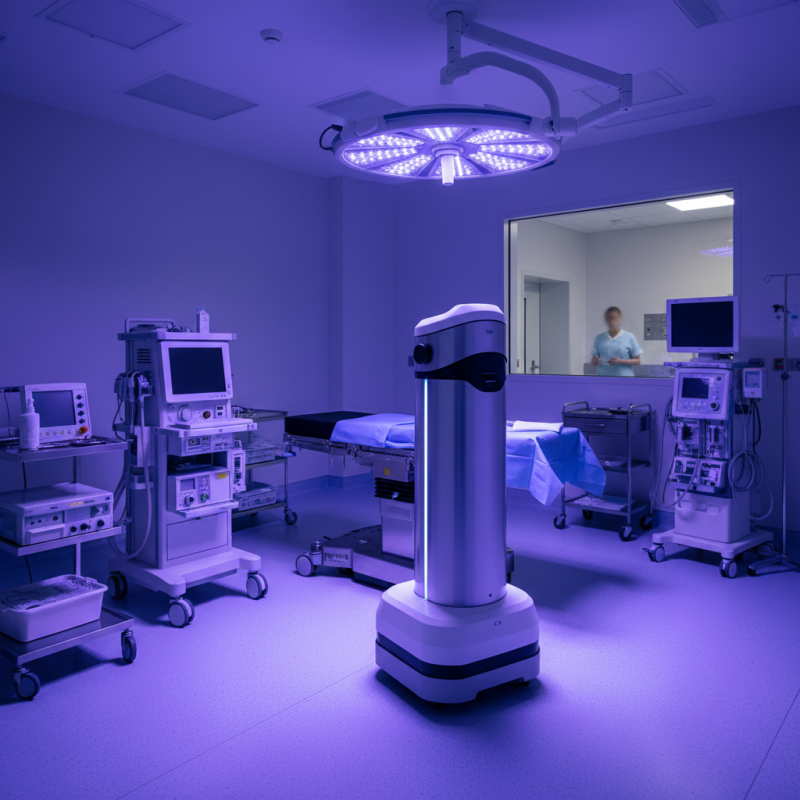
Overview of UV Disinfection Technology in Healthcare Settings
UV disinfection technology is increasingly being adopted in healthcare settings. This method utilizes ultraviolet light to eliminate pathogens. Studies have shown that UV light can deactivate up to 99.9% of certain viruses and bacteria on surfaces. For hospitals, this is crucial. Enhanced patient safety relies on effective infection control.
Tips: Regularly train staff on UV system protocols. Consistent usage can significantly reduce hospital-acquired infections.
Despite its benefits, UV disinfection systems are not foolproof. Shadows can render some areas ineffective. It’s essential to combine UV with traditional cleaning methods. Hospitals must ensure thorough cleaning before UV exposure. Integration of different cleaning techniques can provide the best results.
Tips: Evaluate your facility’s layout. Identify areas at risk of shadowing. Consider additional measures for high-touch surfaces.
The future of healthcare disinfection might revolve around continuous innovation. However, awareness of the limitations of UV technology is necessary. Ongoing assessments and adjustments will be essential. Balancing technology with practical cleaning measures could enhance patient outcomes dramatically.
Top 10 UV Disinfection Systems for Hospitals to Ensure Patient Safety
| System Name | UV Output (mW/cm²) | Coverage Area (sq ft) | Cycle Time (minutes) | Energy Efficiency (W/kWh) |
|---|---|---|---|---|
| System A | 120 | 150 | 5 | 0.15 |
| System B | 110 | 200 | 7 | 0.17 |
| System C | 150 | 180 | 6 | 0.14 |
| System D | 130 | 220 | 4 | 0.16 |
| System E | 140 | 160 | 5 | 0.12 |
| System F | 125 | 190 | 6 | 0.18 |
| System G | 135 | 210 | 4 | 0.13 |
| System H | 145 | 170 | 5 | 0.11 |
| System I | 155 | 230 | 6 | 0.15 |
| System J | 160 | 200 | 5 | 0.19 |
Key Features of Effective UV Disinfection Systems

When it comes to UV disinfection systems in hospitals, key features play a crucial role in ensuring patient safety. Effective systems should be mobile yet sturdy. They need to easily adapt to various hospital settings. Portability allows for flexible use, especially in high-traffic areas. On the other hand, durability ensures that the system can withstand daily operations without frequent repairs.
Another vital aspect is the intensity of UV light. Strong enough intensity kills most pathogens. Hospitals must assess how the UV wavelengths interact with different surfaces. Some areas might require more attention than others. Fast disinfection cycles are crucial too. Time is precious in healthcare. Quick cycling helps maintain efficiency while ensuring thorough disinfection. Hospitals should teach staff on how to use these systems effectively.
Finally, monitoring features are essential for accountability. Disinfection logs should be easily accessible. This improves transparency and helps identify potential failures in the process. Staff must also be trained to recognize signs of malfunction. It is not just about installation; ongoing assessment is necessary. Continuous improvement and reflection on these systems can lead to better patient outcomes.
Comparative Analysis of the Top 10 UV Disinfection Systems
UV disinfection systems are vital for hospitals. They reduce infection rates by targeting pathogens. A study by the Infection Control Society reported that UV light can eliminate up to 99.9% of viruses and bacteria. This effectiveness is crucial for maintaining patient safety in healthcare settings.
When comparing UV disinfection systems, several factors must be considered. The wavelength of UV light, exposure time, and surface coverage are key elements. A comprehensive review revealed that systems using shorter wavelengths, around 254 nm, provided better germicidal action. However, not all designs ensure equal exposure in corners and hidden areas. Some systems face challenges in covering large spaces without resulting in shadows or missed spots.
Moreover, staff training is essential for effective implementation. Misuse can lead to reduced efficacy. A survey indicated that nearly 30% of hospital staff are not fully aware of the proper protocols for operating these systems. This gap can compromise the benefits of UV disinfection. The importance of continuous education cannot be overstated. Balancing technology with trained personnel will enhance patient safety in hospitals.
Top 10 UV Disinfection Systems for Hospitals
This chart illustrates the effectiveness of the top 10 UV disinfection systems based on their disinfection rate (in percentage) and energy consumption (in watts). High disinfection rates and lower energy consumption are optimal for patient safety and operational efficiency.
Benefits of UV Disinfection Systems for Patient Safety
UV disinfection systems have gained recognition in hospitals for their role in enhancing patient safety. According to recent studies, these systems can eliminate up to 99.9% of harmful pathogens. Traditional cleaning methods may leave behind lingering germs. This is a significant concern in healthcare facilities, where infection control is crucial.
One key benefit of UV disinfection is its speed. Unlike chemical disinfectants, UV lights can disinfect a room in just minutes. This rapid turnover can improve efficiency, allowing more patients to be treated promptly. Hospitals that implemented UV systems reported a decline in hospital-acquired infections by approximately 30%. This statistic highlights the effectiveness of UV technology in combating germs.
Tip: Regularly assess the effectiveness of your UV system. Visual inspections can sometimes miss subtle issues. Also, consider your usage frequency for optimal results.
While UV disinfection is effective, it isn’t foolproof. Some pathogens can develop resistance, making continuous evaluation essential. Moreover, UV disinfection should supplement, not replace, routine cleaning practices. Staff training on the safe use of UV systems is equally important. Knowledge gaps can lead to improper usage, diminishing effectiveness.
Tip: Create a protocol for the use of UV equipment. This ensures all staff members operate it correctly and safely. Evaluating protocols regularly helps maintain high safety standards.
Case Studies on UV Disinfection Implementation in Hospitals

In recent years, many hospitals have adopted UV disinfection systems to enhance patient safety. A case study at a large metropolitan hospital showed a 30% reduction in hospital-acquired infections after implementing UV disinfection. Staff noted decreased patient turnover times, but some wondered about the long-term effects on equipment.
Another research study highlighted a smaller facility using UV light to sanitize surgical rooms. Post-implementation data showed improved cleanliness scores but raised questions about the adaptability of staff to new protocols. Changing behaviors was not easy. Training was essential yet time-consuming.
Despite promising results, challenges remain. Hospitals must balance cost and impact. Some facilities reported equipment malfunctions that slowed down workflows. Additionally, effectiveness could vary based on the room size and layout. It’s critical to evaluate these systems continuously to ensure they meet the evolving standards of patient safety.
This website uses cookies to ensure you get the best experience on our website. Learn More
ACCEPT