What is a UV Sterilizer in Medical Equipment and How Does It Work?
In recent years, the use of UV sterilizer medical equipment has gained popularity in healthcare settings. These devices utilize ultraviolet (UV) light to eliminate harmful microorganisms. As a result, they contribute to safer environments for patients and staff alike.
The key mechanism of a UV sterilizer is simple yet effective. When certain wavelengths of UV light hit bacteria or viruses, it disrupts their DNA. This process prevents them from reproducing. The technology is advanced but can sometimes be misunderstood, leading to improper use.
Healthcare facilities must consider the limitations of UV sterilizer medical equipment. Not all surfaces are easily reachable for UV light, reducing effectiveness. Furthermore, improper usage may result in incomplete sterilization. Therefore, a combination of cleaning methods often yields the best results. Understanding these nuances is essential for maximizing safety in medical environments.

What is a UV Sterilizer and Its Role in Medical Equipment?
A UV sterilizer is a crucial device in medical equipment. It uses ultraviolet light to eliminate harmful microorganisms. This process is essential for maintaining a sterile environment in healthcare settings. By effectively killing bacteria and viruses, it helps prevent infections. Units are often small and can be placed in various locations, such as operating rooms or labs.
The method of operation is straightforward. UV lamps emit light at specific wavelengths that disrupt the DNA of germs. Without their DNA, microorganisms cannot reproduce. This makes UV sterilization a powerful tool. However, it is not flawless. Shadows or surfaces that block light can remain contaminated. Regular maintenance and monitoring are important to ensure effectiveness.
Despite its advantages, some practices raise questions. Not all pathogens are equally susceptible to UV light. Some may require longer exposure times. Moreover, over-reliance on UV sterilization can lead to complacency in other cleaning protocols. A balanced approach is vital in infection control.
Understanding the Mechanism of UV-C Light in Sterilization Processes
Ultraviolet (UV) sterilizers use UV-C light to kill germs and pathogens in medical equipment. This specific wavelength of light, ranging from 200 to 280 nanometers, disrupts the DNA of microorganisms. Studies have shown that UV-C can eliminate up to 99.99% of harmful bacteria in just a few seconds. The efficiency of this process is significant, especially in healthcare settings where infection control is paramount.
When UV-C light is applied, it penetrates the cell walls of bacteria and viruses. This leads to the formation of dimers in the DNA, rendering the germs unable to replicate. Many hospitals are now using UV sterilization as a complementary method to traditional cleaning protocols. In fact, a report by the CDC indicates that incorporating UV light can reduce hospital-acquired infections by 30%.
However, the use of UV sterilizers is not without its challenges. Shadows can limit effectiveness; areas not exposed to light may still harbor pathogens. Operators must ensure equipment is placed correctly. Additionally, overuse of UV light may degrade some materials over time. Ongoing research is crucial to refine these methods, balancing efficiency with the longevity of medical instruments.
Effectiveness of UV Sterilizers Against Pathogens: A Statistical Overview
Ultraviolet (UV) sterilizers have gained traction in medical settings for their role in pathogen elimination. These devices use UV light to deactivate microorganisms. They work by altering the DNA or RNA of pathogens. This process prevents the organisms from replicating and ultimately leads to their death. Studies show that UV sterilizers can reduce bacteria and viruses by over 99%.
Statistical data highlights the effectiveness of UV sterilizers. In various tests, these devices demonstrated significant reductions in pathogens, including MRSA and SARS-CoV-2. However, not all UV wavelengths are equally effective. Some wavelengths offer greater pathogen kill rates than others. More research is needed to optimize these variables.
Despite their efficacy, reliance on UV sterilizers can be problematic. They are not a complete solution for sterilization. Operators must consider the shadows created by medical equipment. Areas not exposed to UV light risk harboring pathogens. Furthermore, overexposure to UV light poses safety concerns for workers. Balancing efficacy and safety remains a challenge in medical settings.
Comparison of UV Sterilizers with Traditional Sterilization Methods
UV sterilizers use ultraviolet light to kill bacteria and viruses. This method has gained popularity in the medical field due to its effectiveness. According to research from the American Journal of Infection Control, UV sterilization can reduce microbial populations by up to 99.9% in just a few seconds. This rapid action contrasts with traditional methods, which often require longer exposure times.
Traditional sterilization techniques include steam, dry heat, and chemical processes. While effective, these methods can have downsides. For instance, steam sterilization requires high temperatures and pressures, limiting its application to heat-resistant materials. Chemical methods can leave residues, potentially causing harm to patients. In contrast, UV sterilization is non-invasive and leaves no chemical traces. However, its efficacy can be influenced by the presence of organic matter. If surfaces are not properly cleaned beforehand, UV light may not reach all pathogens.
Despite its advantages, UV sterilization has also been criticized. Some argue that over-reliance on UV methods may lead to a lack of thorough cleaning practices. Additionally, UV light can be harmful to human skin and eyes, posing safety concerns in clinical settings. As we explore these technologies, it's essential to understand their limitations alongside their benefits.
What is a UV Sterilizer in Medical Equipment and How Does It Work? - Comparison of UV Sterilizers with Traditional Sterilization Methods
| Sterilization Method | Mechanism | Advantages | Disadvantages | Typical Applications |
|---|---|---|---|---|
| UV Sterilization | Uses UV-C light to damage DNA/RNA of microorganisms | Fast, chemical-free, effective against viruses and bacteria | Limited penetration, requires direct exposure | Surface disinfection, water purification |
| Autoclave (Steam Sterilization) | Uses steam under pressure to kill microorganisms | Effective for a wide range of pathogens, penetrates porous materials | Requires time to cool down, may damage heat-sensitive items | Surgical instruments, laboratory equipment |
| Ethylene Oxide Sterilization | Uses ethylene oxide gas to sterilize at low temperatures | Effective for heat-sensitive devices, penetrates packaging | Long cycle time, potential toxic residue | Medical devices, electronics |
| Dry Heat Sterilization | Uses hot air to sterilize items through conduction | No moisture damage, effective for oils and powders | Longer exposure time, less efficient than steam | Glassware, metal instruments |
Safety Protocols and Best Practices for Using UV Sterilizers in Healthcare
UV sterilizers play a crucial role in healthcare settings. They use ultraviolet light to kill or inactivate pathogens on surfaces and equipment. However, using these devices requires strict adherence to safety protocols. Staff must wear protective gear to avoid skin and eye exposure. It’s essential to ensure that no one is in the room during the sterilization process, as UV light can cause harm.
Proper positioning is key for effective sterilization. Items must be placed at the right distance from the UV source. Coverage should be thorough to eliminate all potential contaminants. Regular maintenance of the devices is important too. Accumulated dust on the lamps can reduce effectiveness. Inefficient use of these machines may lead to incomplete sterilization. Staff training is vital; understanding the technology ensures that the protocols are followed correctly.
Monitoring the sterilization environment is also necessary. Recording exposure times can help in evaluating the process. It's easy to overlook these details in a busy hospital. Regular audits can identify lapses in protocol adherence. Such reflection can improve overall sterilization practices. An effective use of UV sterilizers can significantly enhance safety in healthcare.
Related Posts
-
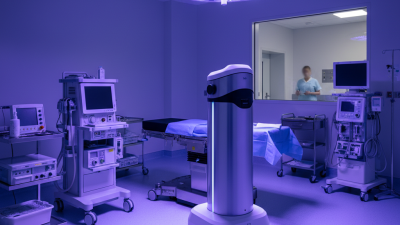
Top 10 UV Disinfection Systems for Hospitals to Ensure Patient Safety?
-
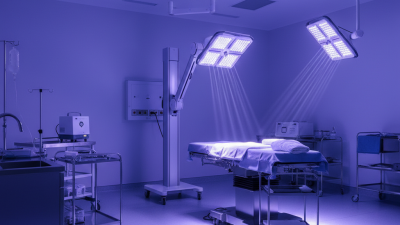
2026 Best Hospital UV Light Disinfection Systems for Improved Safety?
-

Ultimate Tips for Using UVC Light Sterilizer Effectively?
-
Top 10 Best Smart UVC Devices for Effective Disinfection Today?
-

2026 Top Innovations in Infection Prevention Strategies and Technologies?
-
Top 10 UV Light Uses for Sterilization How Effective Is It?
This website uses cookies to ensure you get the best experience on our website. Learn More
ACCEPT