How to Choose the Best UV Sterilizer for Medical Equipment?
In the ever-evolving healthcare landscape, the demand for effective sterilization methods is crucial. Medical facilities prioritize the safety of patients and staff. The "UV sterilizer for medical equipment" stands out as a vital tool. According to a report by the World Health Organization, approximately 1.7 million infections occur in hospitals each year. This alarming statistic highlights the significance of effective sterilization methods.
Dr. Emily Carter, a leading expert in medical sanitation, states, “Choosing the right UV sterilizer can reduce infection rates significantly.” Her insight underlines the impact of selecting appropriate equipment. However, not all UV sterilizers are created equal. Many products on the market fail to meet necessary standards. This inconsistency complicates the decision-making process for healthcare providers.
As practitioners navigate these choices, understanding UV technology becomes essential. Potential users must consider factors such as intensity, wavelength, and material compatibility. The choices available are vast, and missteps in selection can lead to serious consequences. Ensuring proper sterilization is not just a recommendation; it is a necessity for modern medical practice.

Understanding UV Sterilization and Its Importance in Medical Settings
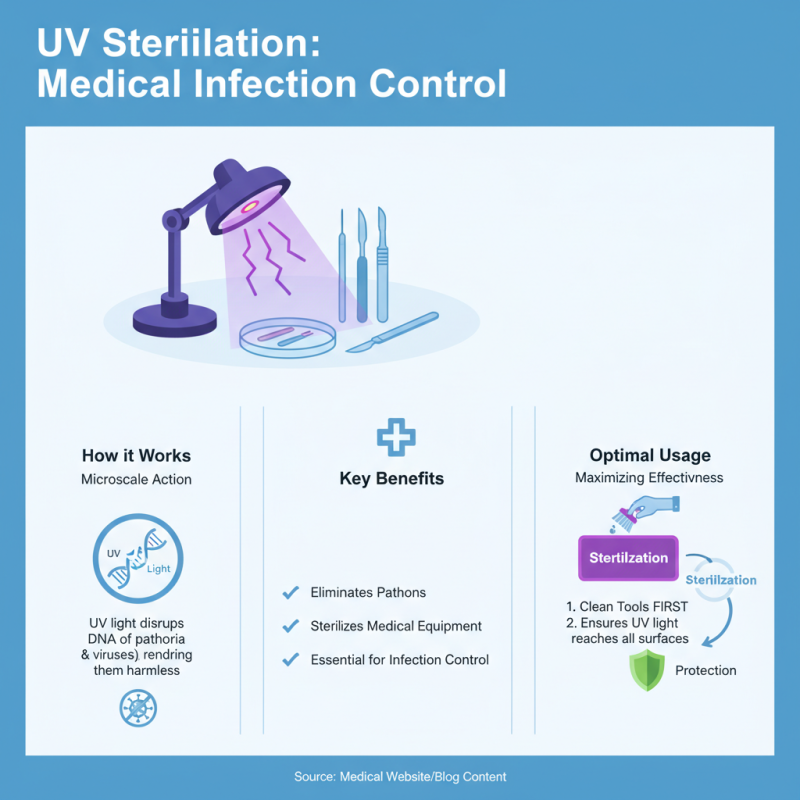
UV sterilization is vital in medical settings. It effectively eliminates pathogens from medical equipment. Understanding how UV light operates is essential for optimal usage. On a micro-scale, UV light disrupts the DNA of bacteria and viruses. This makes it a powerful tool in infection control. Cleaning tools before sterilization enhances UV effectiveness.
Choosing an effective UV sterilizer requires reflection. One must consider the intensity of UV light. Shorter wavelengths offer better germicidal effects. However, overexposure can damage equipment. Balancing efficiency and safety is crucial. Testing different devices can reveal their strengths and weaknesses. Regular maintenance of UV sterilizers is often overlooked. Forgotten bulbs lose their power, leading to ineffective sterilization.
In practice, implementing UV sterilization may face challenges. Personnel might forget to follow protocols. Inconsistent procedures can lead to contamination. Training is necessary, yet often inadequately addressed. Continuous evaluation of sterilization processes ensures they remain effective. Each step, from setup to application, requires attention. This attention to detail fosters a safer medical environment.
Types of UV Sterilizers: Which One Suits Your Needs?
When choosing a UV sterilizer for medical equipment, understanding the types available is crucial. There are mainly three categories:
handheld,
cabinet, and
chamber sterilizers.
Handheld sterilizers are portable. They are ideal for small tools and surfaces. However, their effectiveness depends on user technique. A slight oversight can result in missed areas, reducing sterilization efficiency.
Cabinet sterilizers offer more space. They can accommodate larger equipment. Users appreciate the ease of use; simply place items inside and close the door. Yet, they may lack versatility. Not every cabinet can handle all types of materials. Make sure to check compatibility before making a decision.
Chamber sterilizers are advanced. They provide thorough exposure to UV light. However, their size can be a drawback. Not every facility has the space for these units. Additionally, maintenance is critical. Regular checks are necessary to ensure optimal performance. Neglecting this could lead to issues. Ultimately, considering your specific needs is vital.
Assessing your equipment, space, and user habits will guide you to the best choice.
Key Features to Look for When Choosing a UV Sterilizer
When choosing a UV sterilizer for medical equipment, several key features should be prioritized. One of the most critical aspects is the wavelength of the UV light. Generally, a wavelength between 200 to 280 nanometers is most effective for killing bacteria and viruses. Ensure the sterilizer emits UVC light, as this frequency has proven efficacy against pathogens in medical environments.
Another vital feature is the coverage area. A larger UV chamber may speed up the process, as it can accommodate more items at once. Look for sterilizers that allow you to adjust the time and distance of exposure. This flexibility is crucial, as different materials might require varying exposure levels.
Consider the portability of the device as well. Mobile sterilizers make it easier to sanitize equipment outside traditional settings. However, take note that a more compact design may reduce effectiveness. Additionally, while most UV sterilizers come with safety features, double-check that the device automatically shuts off when opened. Inadequate safety measures could lead to potential harm. Ultimately, these thoughtful details will ensure selecting an effective UV sterilizer for your needs.
Evaluating Effectiveness: UV Intensity and Exposure Time
When considering a UV sterilizer for medical equipment, evaluating UV intensity is crucial. Not all devices emit the same level of UV light. The intensity determines how effectively pathogens are eliminated. A higher intensity might seem better, but can it harm some materials? This is a key question. Many sterilizers operate at various UV wavelengths, each targeting different microorganisms.
Exposure time is another critical factor. Longer exposure may seem beneficial, but it can lead to equipment degradation. How long is long enough without causing damage? Ideally, tests should be conducted using markers or indicators to evaluate effectiveness. Finding the right balance between intensity, exposure time, and equipment safety is not straightforward.
Moreover, consider the environment where sterilization occurs. Dust or obstructions can significantly impact the process. Regular maintenance of the device is essential. Without proper upkeep, the effectiveness can diminish over time. Ensuring consistent performance often requires an ongoing assessment. This continuous evaluation can sometimes feel overwhelming but is necessary for optimal results.
How to Choose the Best UV Sterilizer for Medical Equipment? - Evaluating Effectiveness: UV Intensity and Exposure Time
| Sterilizer Type | UV Intensity (mW/cm²) | Exposure Time (minutes) | Effective Dose (mJ/cm²) | Application |
|---|---|---|---|---|
| Handheld UV Sterilizer | 45 | 5 | 225 | Surface Disinfection |
| UV Chamber Sterilizer | 100 | 10 | 1000 | Instrument Sterilization |
| UV Conveyor Sterilizer | 80 | 8 | 640 | Continuous Flow Disinfection |
| Portable UV Sterilizer | 50 | 7 | 350 | Small Equipment Disinfection |
Safety Considerations in Using UV Sterilizers for Medical Equipment
When selecting a UV sterilizer for medical equipment, safety should be a top priority. UV-C light effectively eliminates pathogens, but it can also pose risks to users and patients if not handled properly. Studies show that UV-C light can cause skin burns and eye damage. Protecting staff is essential. Equip sterilization areas with appropriate shields. Proper personal protective equipment (PPE) must be worn during operation.
Monitoring exposure time and distance is crucial. Research indicates that UV-C effectiveness decreases significantly beyond three feet. Many sterilizers have features like automatic shut-off and timers. These can enhance safety but are not foolproof. Regular training on best practices can help staff understand the risks. Inconsistent protocols can lead to neglecting safety measures, increasing the risk of harmful exposure.
Validation of the sterilization process is also important. Regular testing with biological indicators ensures that equipment is effectively sterilized. The American Journal of Infection Control emphasizes the need for routine checks. Equipment failures can occur. Operators should remain vigilant and report any anomalies immediately. The reality is that reliance solely on UV sterilization without appropriate safety measures can be a significant oversight in any healthcare setting.
Related Posts
-
Top 10 UV Light Uses for Sterilization How Effective Is It?
-
Top 10 Best Smart UVC Devices for Effective Disinfection Today?
-

2026 Top UV Disinfection System for Hospitals What to Expect?
-
Top 10 UV Disinfection Systems for Hospitals to Ensure Patient Safety?
-

What is a UV Sterilizer in Medical Equipment and How Does It Work?
-
2026 Best Hospital UV Light Disinfection Systems for Improved Safety?
This website uses cookies to ensure you get the best experience on our website. Learn More
ACCEPT